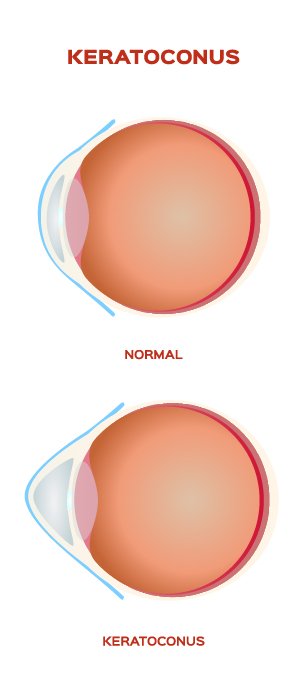
The cornea is the window of the eye. Light travels through the cornea past the lens to the retina and then the brain to form a visual image. The normal corneal surface is smooth and aspheric i.e. round in the center, flattening towards its outer edges. Light rays passing through it moves in an undistorted manner to the retina to project a clear image to the brain.
In patients with keratoconus the cornea is cone shaped (hence the name keratoconus, derived from the greek word for cornea (‘kerato’) and cone shaped (‘conus’). In patients with keratoconus the cornea is not only cone shaped but the surface is also irregular resulting in a distorted image being projected onto the brain.
Keratoconus typically commences at puberty and progresses to the mid-thirties at which time progression slows and often stops. Between ages 12 and 35 it can arrest or progress at any time and there is now way to predict how fast it will progress or if it will progress at all. In general, young patients with advanced disease are more likely to progress to the point where they may ultimately require some form of surgical intervention.
Keratoconus may occur in one eye only initially but most commonly affects both eyes with one eye being more severely affected than the other. Both males and females are equally affected.